Medicare
-
Comparing Commercial and Medicare Professional Service Prices
 Read more: Comparing Commercial and Medicare Professional Service Prices
Read more: Comparing Commercial and Medicare Professional Service PricesPeople in the United States routinely cite health care and health care costs as top concerns.1,2,3,4 For the more than 160 million people who get insurance from their employer, the cost of health care is high, growing, and outpacing growth in wages.5,6,7 Across the country, health care costs show up in the form of higher premiums and…
-
Commercial Prices Relative to Medicare Vary Within Metro Areas Across Specialties and by Type of Service
 Read more: Commercial Prices Relative to Medicare Vary Within Metro Areas Across Specialties and by Type of Service
Read more: Commercial Prices Relative to Medicare Vary Within Metro Areas Across Specialties and by Type of ServiceEarlier HCCI research found that at the national level, commercial payers paid prices that were, on average, 122% of Medicare. However, we found that commercial professional service prices varied dramatically across states from 98% of Medicare in Alabama to 188% of Medicare in Wisconsin. There was similar variation within states, such as California, and also…
-
Charge Amounts for Professional Procedures to Commercial Insurance and Traditional Medicare
 Read more: Charge Amounts for Professional Procedures to Commercial Insurance and Traditional Medicare
Read more: Charge Amounts for Professional Procedures to Commercial Insurance and Traditional MedicareIn the start of 2019, Centers for Medicare and Medicaid Services finalized federal policies that required hospitals to publish the amount they charge for common services, documents commonly referred to as chargemasters. While similar policies have been in place at the state level since the early 2000s, this was the first federal mandate to require…
-
ADRD Prevalence in Various Insurance Populations: A Collaboration with The Alzheimer’s Association
 Read more: ADRD Prevalence in Various Insurance Populations: A Collaboration with The Alzheimer’s Association
Read more: ADRD Prevalence in Various Insurance Populations: A Collaboration with The Alzheimer’s AssociationAlzheimer’s disease and related dementias (ADRD) represent a significant and growing cost to the United States health care system. While the prevalence and cost of ADRD related to Medicare Fee-for-Service beneficiaries is documented in the Center for Medicare and Medicaid Services’ Chronic Conditions Warehouse, less is known about the prevalence and cost of ADRD among…
-
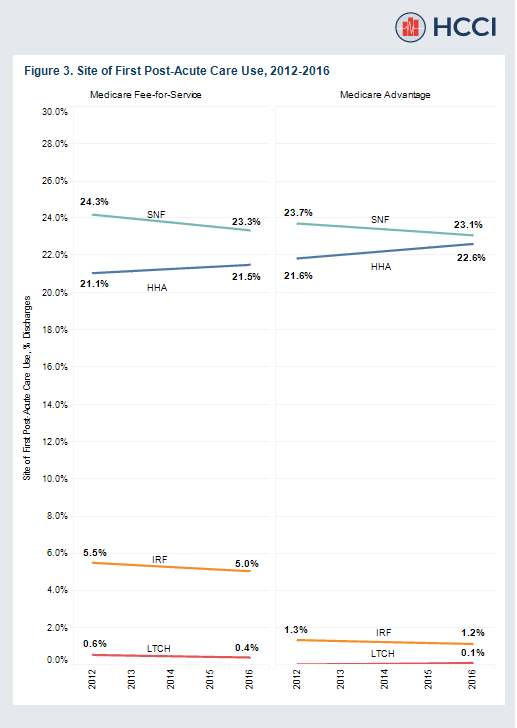
Comparing Post-Acute Care Use and First Site of Care Among Medicare Advantage Enrollees and Medicare Fee-for-Service Beneficiaries
Read more: Comparing Post-Acute Care Use and First Site of Care Among Medicare Advantage Enrollees and Medicare Fee-for-Service BeneficiariesUsing data from the Health Care Cost Institute (HCCI) and Centers for Medicare & Medicaid Services (CMS), we examined trends in inpatient hospital admissions and post-acute care (PAC) utilization among Medicare Advantage (MA) and Fee-for-Service (FFS) beneficiaries. Specifically, we compared how frequently individuals in each group were discharged from the hospital, whether they had evidence…
-
Comparing Average Rates for Select Anesthesiology, Emergency Medicine, and Radiology Services by Local Areas
Tags: Commercially Insured, Emergency Room, Geographic Variation, Medicare, Out-of-Network, Physician SpendingRead more: Comparing Average Rates for Select Anesthesiology, Emergency Medicine, and Radiology Services by Local AreasWhen a person unknowingly receives health care services from a provider that is outside of their insurer’s network, it gives rise to the potential for a “surprise bill”. Congress continues to consider legislation aimed at reducing the financial burden of “surprise bills” for patients. The approach approved by committees in both the House and Senate…
-
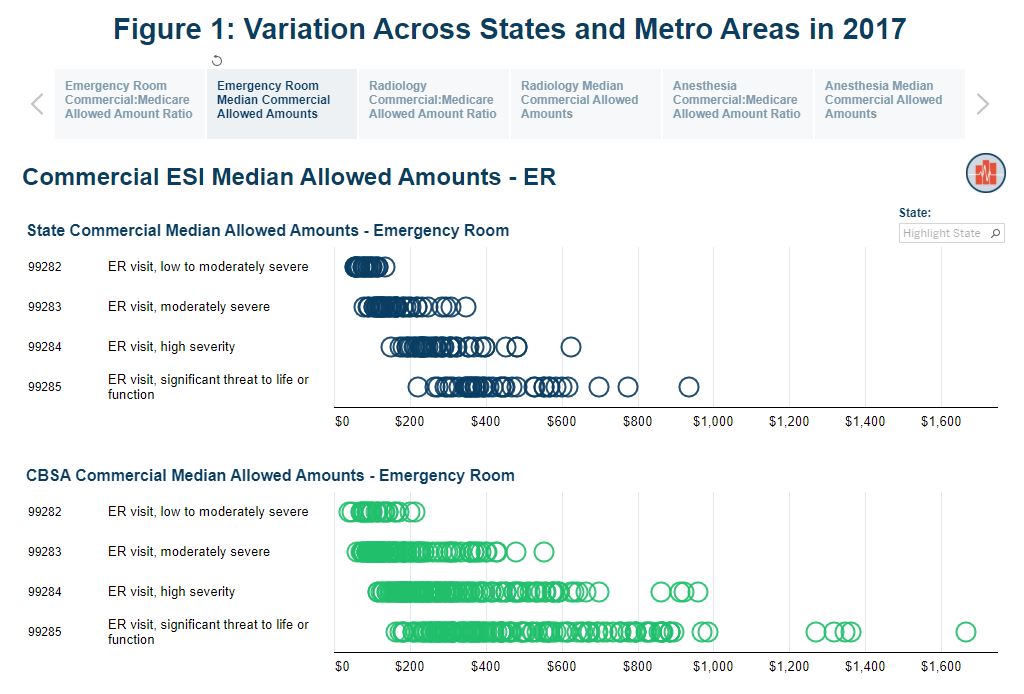
Comparing Commercial and Medicare Rates for Select Anesthesia, Emergency Room, and Radiology Services by State
Tags: Commercially Insured, Emergency Room, Medicare, Physician Spending, Prices, Spending, Surprise Billing Read more: Comparing Commercial and Medicare Rates for Select Anesthesia, Emergency Room, and Radiology Services by State
Read more: Comparing Commercial and Medicare Rates for Select Anesthesia, Emergency Room, and Radiology Services by StateCommittees in both the House and Senate have advanced legislation that includes measures to address “surprise bills.” A surprise bill results when a person unknowingly receives medical care from a provider that is not part of their insurer’s network. Both pieces of legislation set a benchmark for out-of-network payments. Those benchmarks are determined based on…
-
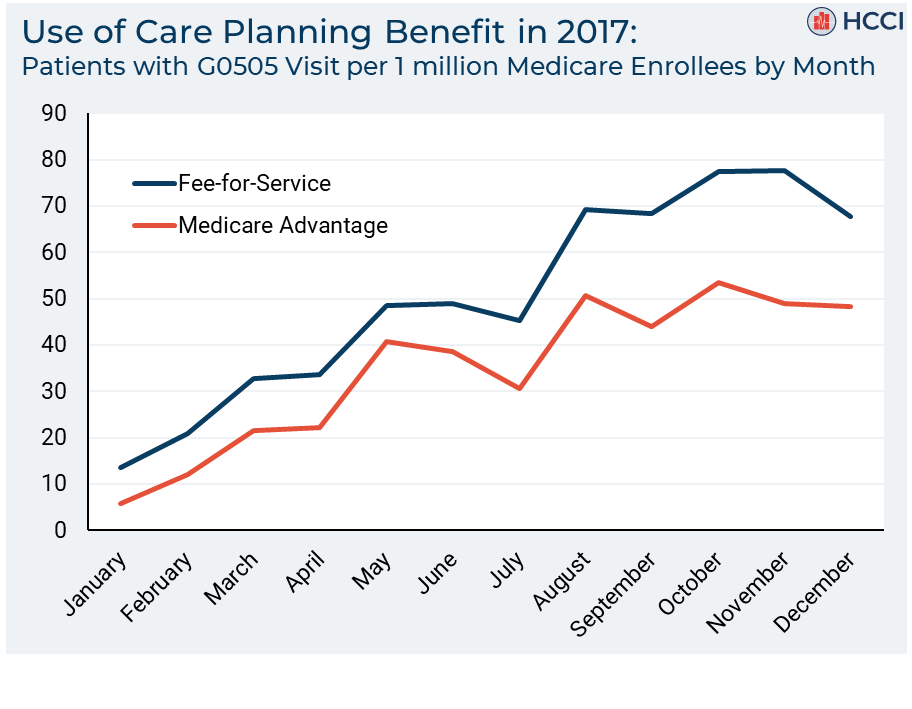
Examining the adoption of a new Medicare billing code for cognitive assessments: a slow but steady uptake
 Read more: Examining the adoption of a new Medicare billing code for cognitive assessments: a slow but steady uptake
Read more: Examining the adoption of a new Medicare billing code for cognitive assessments: a slow but steady uptakeOn January 1, 2017, the Medicare program started reimbursing providers for a new procedure code for clinical visits for cognitive assessments and care planning services (CPT code G0505). This newly-billable service is intended to improve the care of patients with Alzheimer’s disease and related dementias and hopefully increase early detection and diagnosis. A G0505 visit…
-
Health Affairs: Medicare Competitive Bidding Program Realized Price Savings For Durable Medical Equipment Purchases
 Read more: Health Affairs: Medicare Competitive Bidding Program Realized Price Savings For Durable Medical Equipment Purchases
Read more: Health Affairs: Medicare Competitive Bidding Program Realized Price Savings For Durable Medical Equipment PurchasesABSTRACT: From the inception of the Medicare program there have been questions regarding whether and how to pay for durable medical equipment, prosthetics, orthotics, and supplies. In 2011 the Centers for Medicare and Medicaid Services (CMS) implemented a competitive bidding program to reduce spending on durable medical equipment and similar items. Previously, CMS had used…