Peer Reviewed Journals
-
JAMA Research Letter: Primary Care Spending in the Commercially Insured Population
 Read more: JAMA Research Letter: Primary Care Spending in the Commercially Insured Population
Read more: JAMA Research Letter: Primary Care Spending in the Commercially Insured PopulationUsing HCCI’s data, we assessed the share among individuals younger than 65 years covered by employer-sponsored insurance from 2013 to 2017. We assessed primary care spending using 2 main definitions: a definition which included the total spending on services rendered by primary care clinicians (broad definition) and one where only CPT codes for specific services specified as…
-
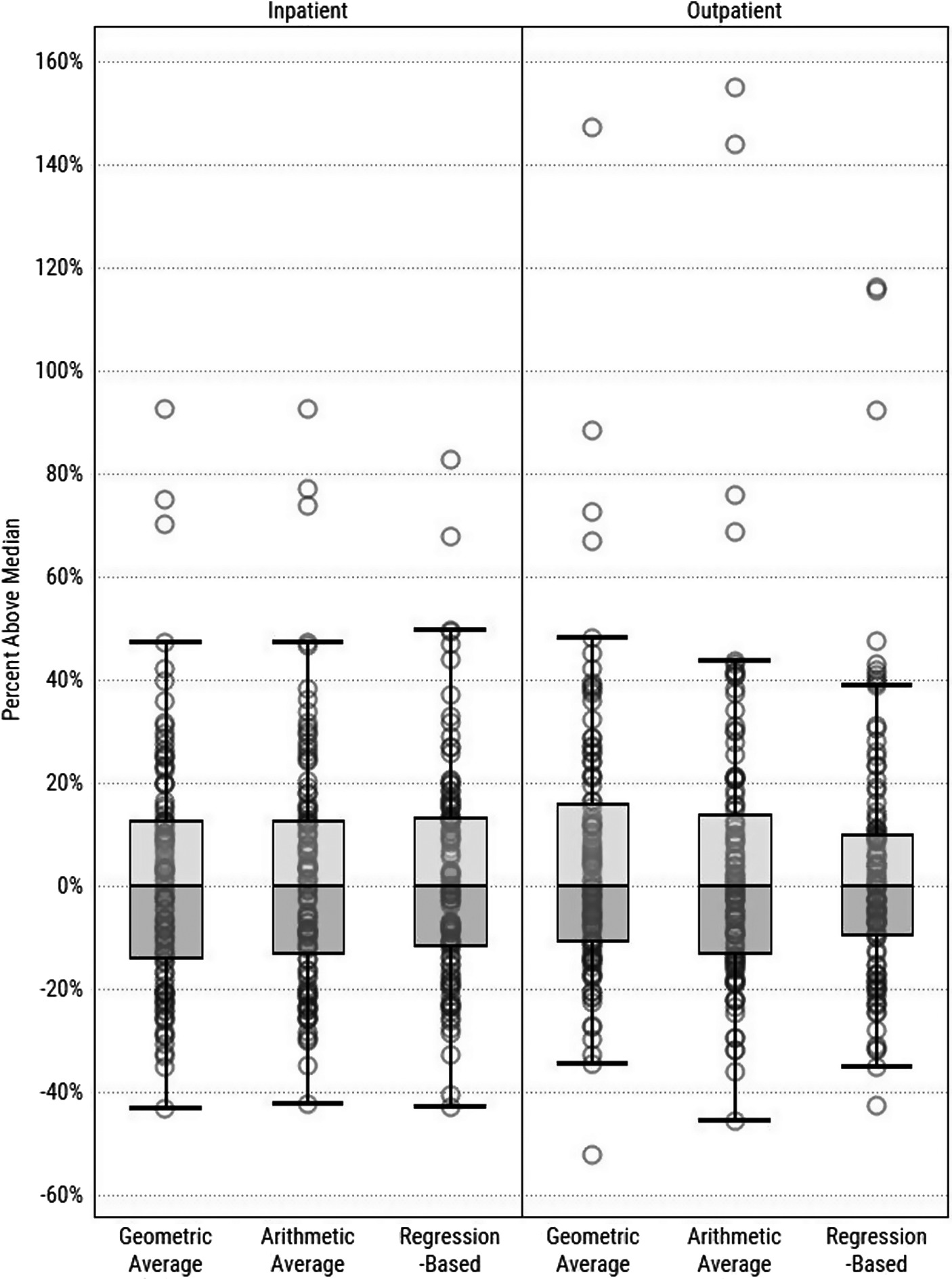
Health Services Research: Comparing Different Methods of Indexing Commercial Health Care Prices
 Read more: Health Services Research: Comparing Different Methods of Indexing Commercial Health Care Prices
Read more: Health Services Research: Comparing Different Methods of Indexing Commercial Health Care PricesThe methodology for HCCI’s Healthy Marketplace Index was published in a Methods Brief for Health Services Research. Abstract Objective: To compare different methods of indexing health care service prices for the commercially insured population across geographic markets. Data Sources: Health Care Cost Institute commercial claims data from 2012 to 2016. Study Design: We compare price indices computed using…
-
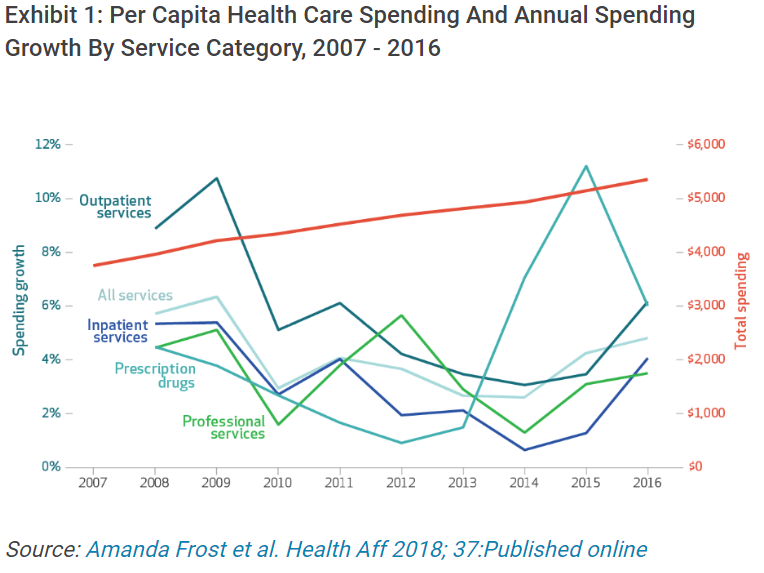
Health Affairs: Health Care Spending Under Employer-Sponsored Insurance: A 10-Year Retrospective
Tags: Commercially Insured, Drug Spending, Health Affairs, Inpatient Spending, Outpatient Spending, Peer Reviewed Journals, Physician SpendingRead more: Health Affairs: Health Care Spending Under Employer-Sponsored Insurance: A 10-Year RetrospectiveABSTRACT Using a national sample of health care claims data from the Health Care Cost Institute, we found that total spending per capita (not including premiums) on health services for enrollees in employer-sponsored insurance plans increased by 44 percent from 2007 through 2016 (average annual growth of 4.1 percent). Spending increased across all major categories…
-
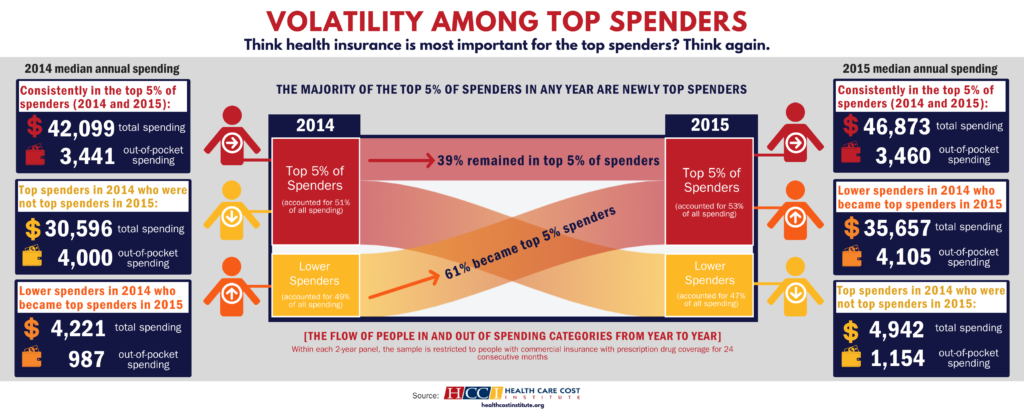
New England Journal of Medicine: Consistently High Turnover in the Group of Top Health Care Spenders
 Read more: New England Journal of Medicine: Consistently High Turnover in the Group of Top Health Care Spenders
Read more: New England Journal of Medicine: Consistently High Turnover in the Group of Top Health Care SpendersNEJM CATALYST: “The concentration of most U.S. health care spending in a small proportion of individuals is well documented. The notion that high health care spending only affects a small portion of people in a given year is particularly relevant to the ongoing policy debate about how to make health insurance affordable for all, while…
-
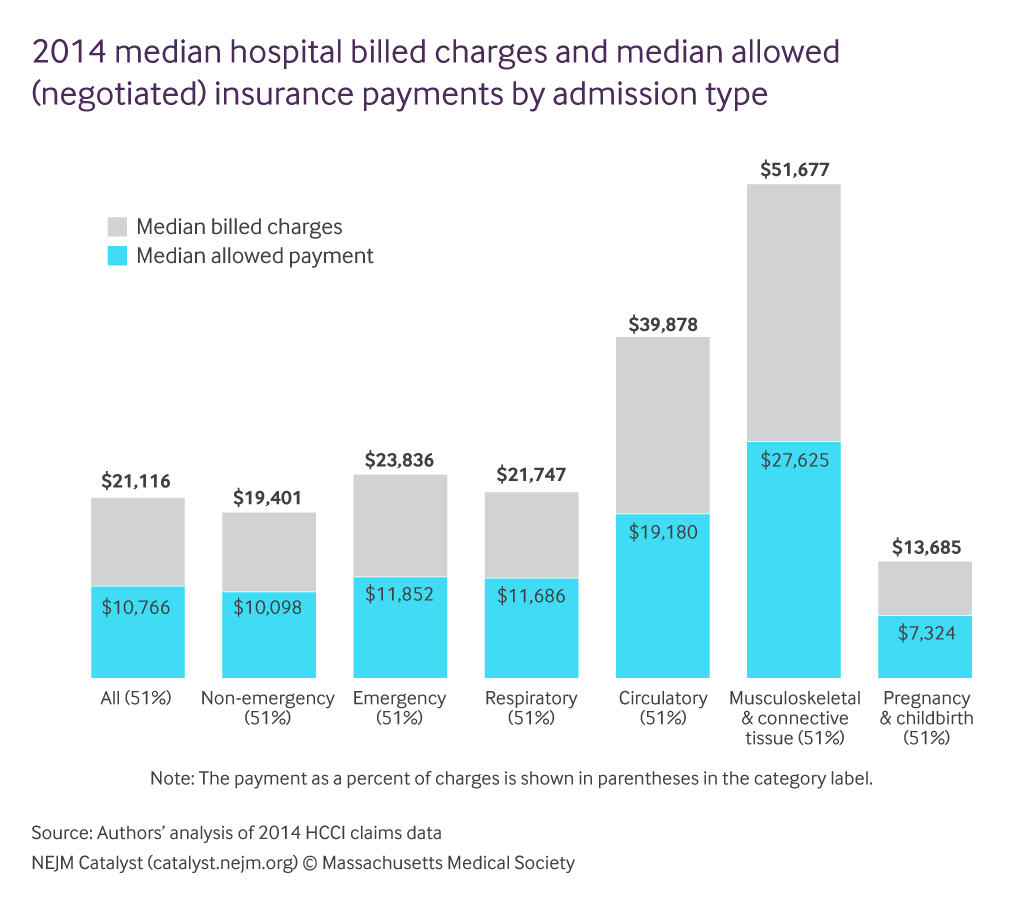
New England Journal of Medicine: The Value of Health Insurance through Price Discounts
 Read more: New England Journal of Medicine: The Value of Health Insurance through Price Discounts
Read more: New England Journal of Medicine: The Value of Health Insurance through Price DiscountsNEJM CATALYST: “As context for the ongoing health care reform debate, we analyzed Health Care Cost Institute (HCCI) data. HCCI is a nonpartisan, nonprofit organization aimed at providing complete and accurate information about health care utilization and costs in the United States. Our goal was to demonstrate the value of insurance through these discounted rates.…
-
JAMA Internal Medicine: A Perspective on Out-of-Pocket Spending
 Read more: JAMA Internal Medicine: A Perspective on Out-of-Pocket Spending
Read more: JAMA Internal Medicine: A Perspective on Out-of-Pocket SpendingTo the Editor Understanding out-of-pocket spending is critical to understanding health care costs in the United States. We applaud the efforts of Adrion et al as an important contribution to understanding the out-of-pocket spending of the commercially insured population younger than 65 years. The commercially insured comprise over 50% of the nonelderly US population and, as…
-
American Journal of Managed Care: Overcoming barriers to a research-ready national commercial claims database
 Read more: American Journal of Managed Care: Overcoming barriers to a research-ready national commercial claims database
Read more: American Journal of Managed Care: Overcoming barriers to a research-ready national commercial claims databaseABSTRACT Objectives: Billions of dollars have been spent on the goal of making healthcare data available to clinicians and researchers in the hopes of improving healthcare and lowering costs. However, the problems of data governance, distribution, and accessibility remain challenges for the healthcare system to overcome. Study Design: In this study, we discuss some of the…
-
Health Affairs: Trends Underlying Employer-Sponsored Health Insurance Growth For Americans Younger Than Age Sixty-Five
 Read more: Health Affairs: Trends Underlying Employer-Sponsored Health Insurance Growth For Americans Younger Than Age Sixty-Five
Read more: Health Affairs: Trends Underlying Employer-Sponsored Health Insurance Growth For Americans Younger Than Age Sixty-FiveABSTRACT Little is known about the trends in health care spending for the 156 million Americans who are younger than age sixty-five and enrolled in employer-sponsored health insurance. Using a new source of health insurance claims data, we estimated per capita spending, utilization, and prices for this population between 2007 and 2011. During this period…