All HCCI Reports
HCCI’s original reports powered by #HCCIdata
-
How common is out-of-network billing?
Tags: Commercially Insured, Emergency Room, Geographic Variation, Mental Health and Substance Use, Out-of-Network, Surprise Billing Read more: How common is out-of-network billing?
Read more: How common is out-of-network billing?Congress is considering legislation to address “surprise bills”, which occur when a person visits an in-network facility, but receives services from a provider that is outside of their insurer’s network. Bills in both the House and Senate include provisions to determine a benchmark rate for out-of-network payments based on what in-network providers of the same…
-
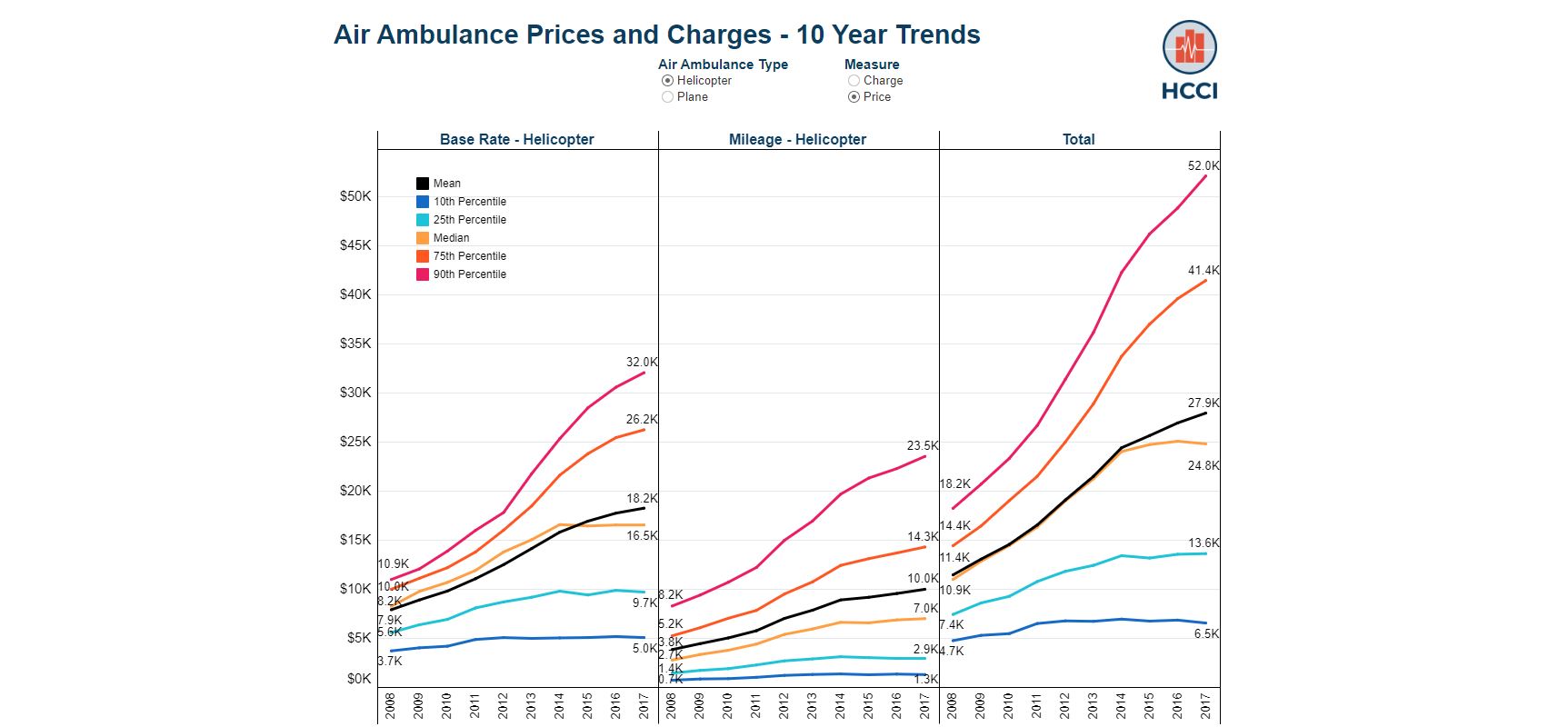
Air Ambulances – 10 Year Trends in Costs and Use
Tags: 10 Year Trend, Ambulance, Charges, Commercially Insured, Emergency Room, Outpatient Spending, Prices, UtilizationRead more: Air Ambulances – 10 Year Trends in Costs and UseAir ambulances are either fixed wing (airplane) or rotary wing (helicopter) aircraft used to transport people in often time-sensitive medical situations. Air ambulances have become a frequent topic in the news due to their high cost and propensity to lead to surprise bills. Our analysis shows that although air ambulances are not frequently used and…
-
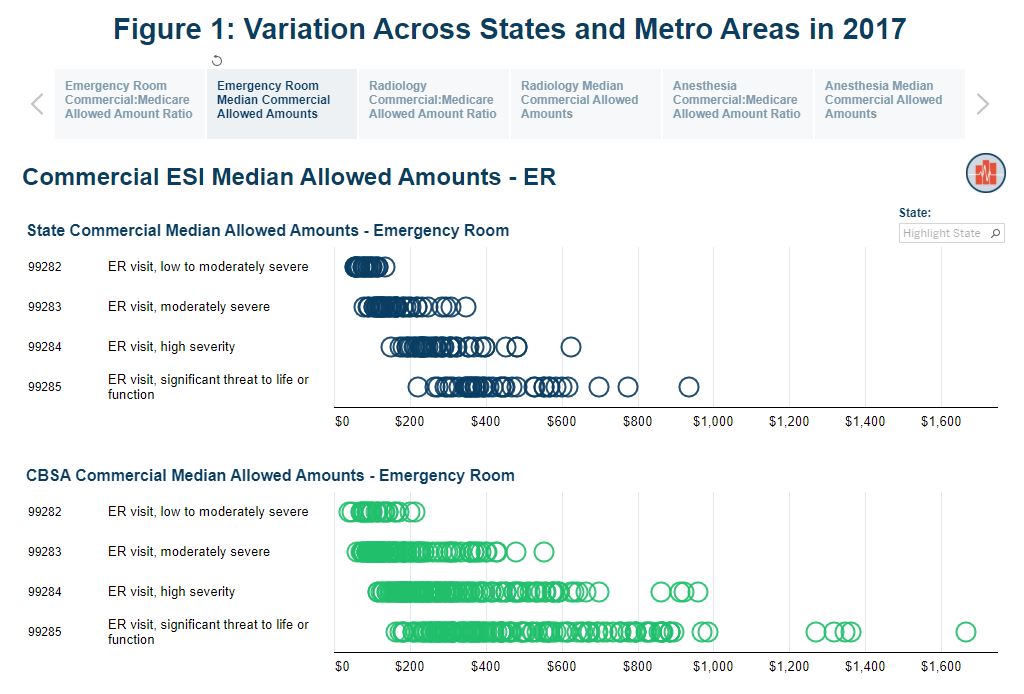
Comparing Average Rates for Select Anesthesiology, Emergency Medicine, and Radiology Services by Local Areas
Tags: Commercially Insured, Emergency Room, Geographic Variation, Medicare, Out-of-Network, Physician SpendingRead more: Comparing Average Rates for Select Anesthesiology, Emergency Medicine, and Radiology Services by Local AreasWhen a person unknowingly receives health care services from a provider that is outside of their insurer’s network, it gives rise to the potential for a “surprise bill”. Congress continues to consider legislation aimed at reducing the financial burden of “surprise bills” for patients. The approach approved by committees in both the House and Senate…
-
Antidepressant Use Increased for Individuals with a Mood Disorder with Employer-Sponsored Insurance
 Read more: Antidepressant Use Increased for Individuals with a Mood Disorder with Employer-Sponsored Insurance
Read more: Antidepressant Use Increased for Individuals with a Mood Disorder with Employer-Sponsored InsuranceDepression is a common mood disorder that affects how people feel, think, and conduct daily activities. Approximately 17 million adults (1 in 14) had at least one major depressive episode in 2017. Surveys have found that antidepressant prescribing has increased over the past two decades. For example, a 2017 National Center for Health Statistics survey found that,…
-
Insulin Use Explains Variation in Level, but not Growth, of Out-of-Pocket Spending on Insulin Products
 Read more: Insulin Use Explains Variation in Level, but not Growth, of Out-of-Pocket Spending on Insulin Products
Read more: Insulin Use Explains Variation in Level, but not Growth, of Out-of-Pocket Spending on Insulin ProductsWe previously published two blogs discussing trends in out-of-pocket spending on insulin products. First, we presented data illustrating how average monthly out-of-pocket spending in 2017 varied considerably by month, particularly for individuals enrolled in consumer-directed health plans (CDHPs) that carry higher deductibles. Second, we examined the relationship between increasing point-of-sale prices between 2012 and 2017…
-
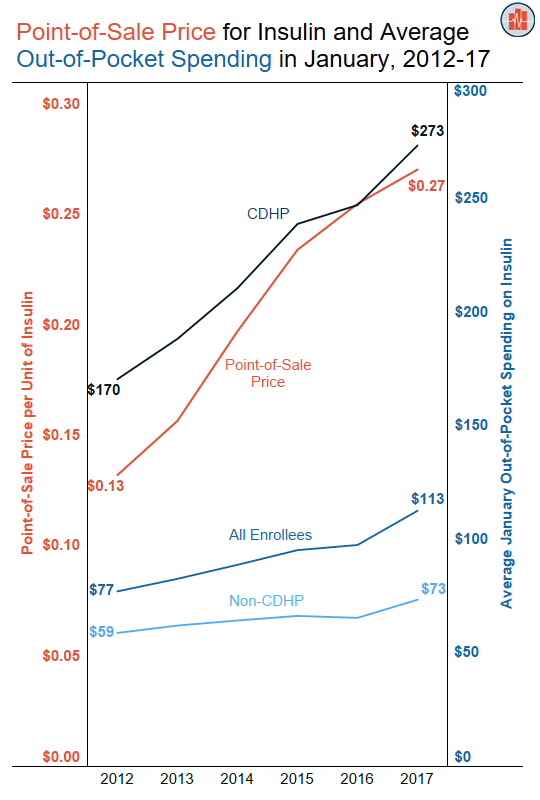
Rising Point-of-Sale Prices for Insulin Correspond with Higher Out-of-Pocket Spending on Insulin in January
 Read more: Rising Point-of-Sale Prices for Insulin Correspond with Higher Out-of-Pocket Spending on Insulin in January
Read more: Rising Point-of-Sale Prices for Insulin Correspond with Higher Out-of-Pocket Spending on Insulin in JanuaryEarlier this week we presented data on out-of-pocket spending on insulin during each month in 2017. In that blog, we showed that enrollees in employer-sponsored health insurance paid more out-of-pocket for insulin products at the beginning of the calendar year. We examined the relationship between increasing point-of-sale prices for insulin and higher out-of-pocket spending in…
-
Out-of-Pocket Spending on Insulin is Highest at the Beginning of the Year
Tags: Commercially Insured, Consumer-Directed Health Plans, Diabetes, Drug Spending, Geographic Variation, Insulin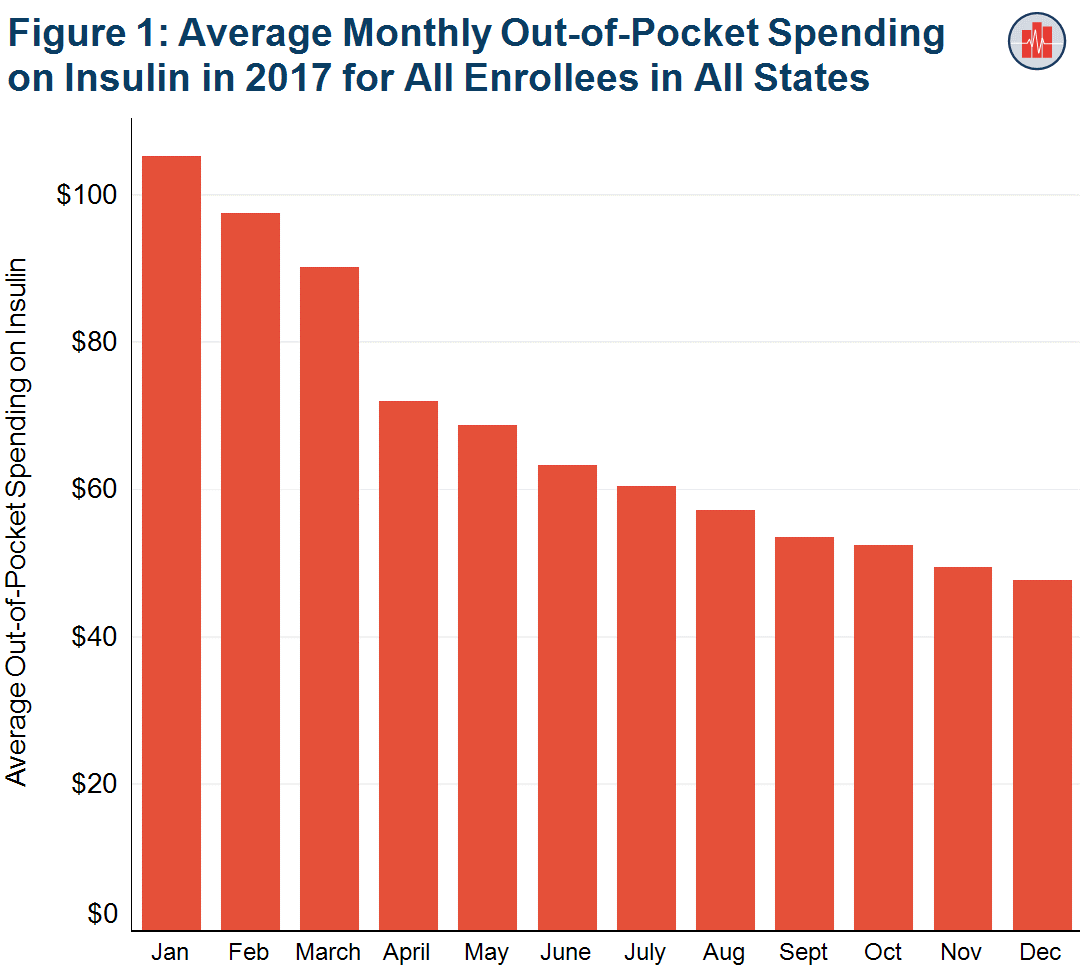 Read more: Out-of-Pocket Spending on Insulin is Highest at the Beginning of the Year
Read more: Out-of-Pocket Spending on Insulin is Highest at the Beginning of the YearPeople who get health insurance through their jobs pay more than twice as much for insulin at the beginning of the year than they do at the end of the year, on average. New analysis of HCCI data shows that, nationally, in January 2017, average out-of-pocket spending on insulin was $105. This spending declined every…
-
State Variation in Opioid Prescribing over 10 Years
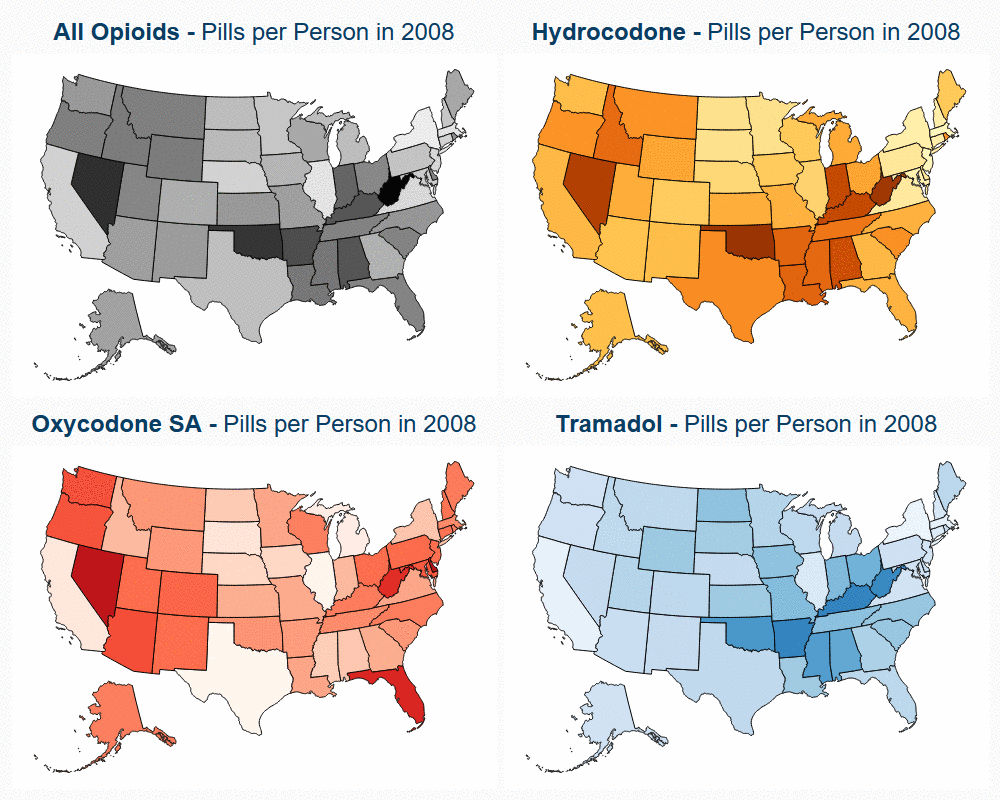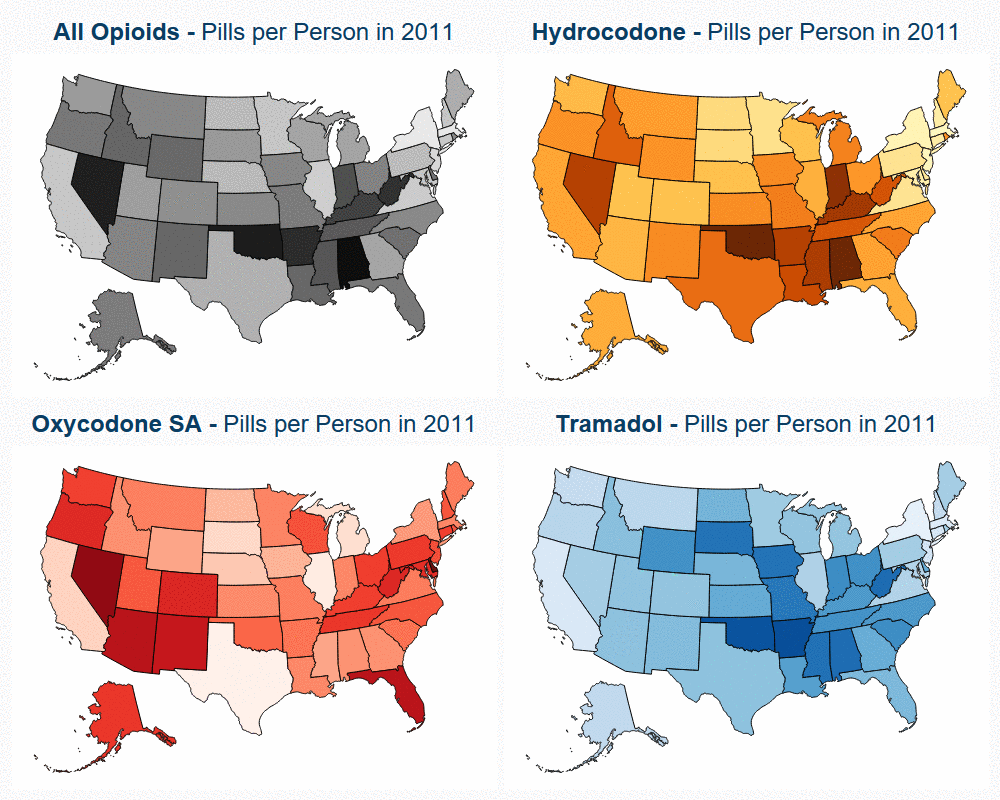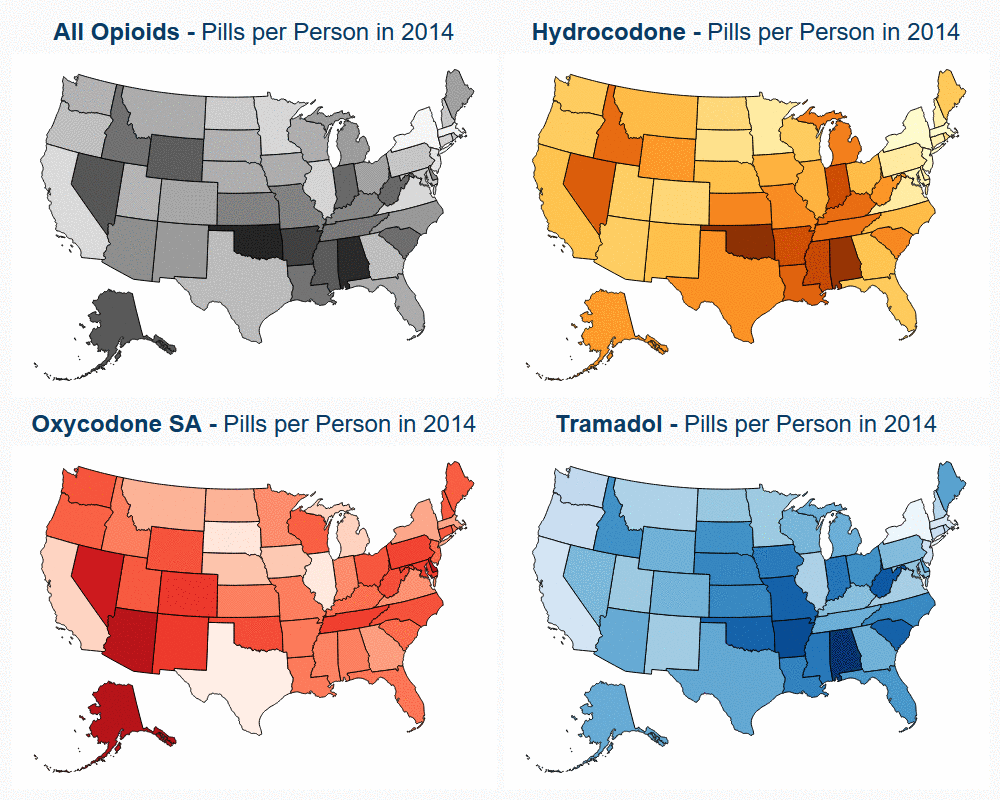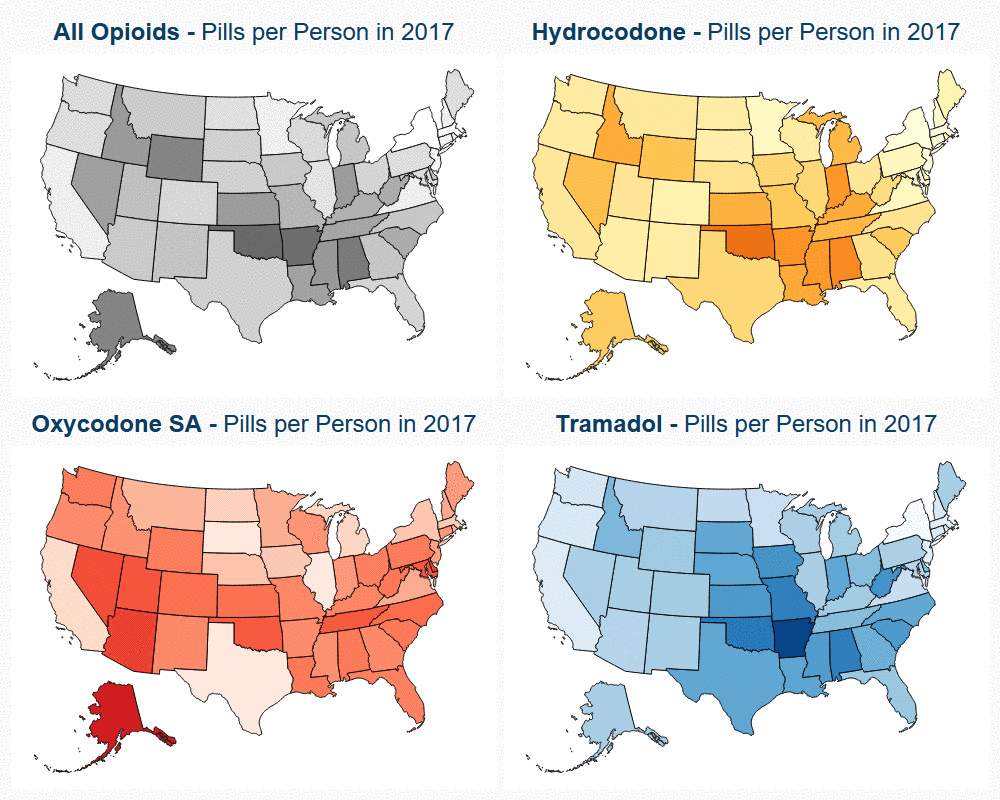 Read more: State Variation in Opioid Prescribing over 10 Years
Read more: State Variation in Opioid Prescribing over 10 YearsChanges in opioid utilization correlated with state-level policy changes aimed at decreasing opioid prescription rates. Previous research by HCCI illustrated that national opioid utilization in pills per person fell 27% between the years of 2008 and 2017, driven by declines in the use of hydrocodone (Vicodin). In addition to giving insight into prescription opioid utilization…
-
Comparing Commercial and Medicare Rates for Select Anesthesia, Emergency Room, and Radiology Services by State
Tags: Commercially Insured, Emergency Room, Medicare, Physician Spending, Prices, Spending, Surprise Billing Read more: Comparing Commercial and Medicare Rates for Select Anesthesia, Emergency Room, and Radiology Services by State
Read more: Comparing Commercial and Medicare Rates for Select Anesthesia, Emergency Room, and Radiology Services by StateCommittees in both the House and Senate have advanced legislation that includes measures to address “surprise bills.” A surprise bill results when a person unknowingly receives medical care from a provider that is not part of their insurer’s network. Both pieces of legislation set a benchmark for out-of-network payments. Those benchmarks are determined based on…
-
Opioid Prescriptions Declined 32% for the Commercially Insured over 10 Years (2008 to 2017)
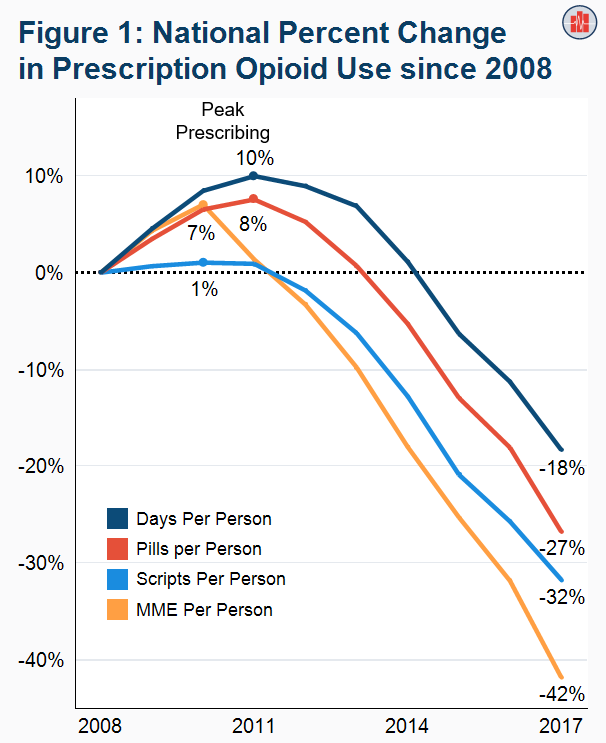 Read more: Opioid Prescriptions Declined 32% for the Commercially Insured over 10 Years (2008 to 2017)
Read more: Opioid Prescriptions Declined 32% for the Commercially Insured over 10 Years (2008 to 2017)Among people who get health insurance from their employers (56% of the population in 2017), prescription opioid use peaked in 2010/2011 and declined every year from 2012 to 2017. In a new study using the Health Care Cost Institute’s commercial claims data from 2008 to 2017, we observed a decline regardless of how utilization was…