Topics
Out-of-Pocket Spending on Insulin is Highest at the Beginning of the Year
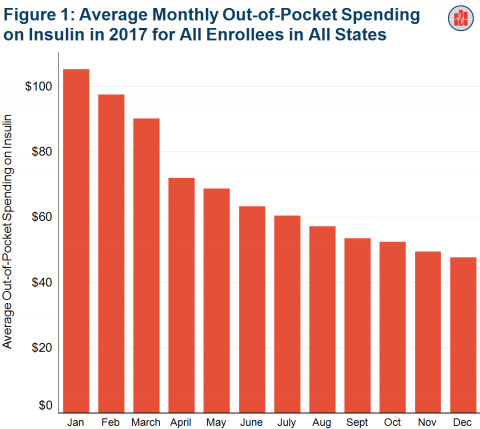
People who get health insurance through their jobs pay more than twice as much for insulin at the beginning of the year than they do at the end of the year, on average. New analysis of HCCI data shows that, nationally, in January 2017, average out-of-pocket spending on insulin was $105. This spending declined every month throughout the calendar year, likely as enrollees met their annual deductible, and in December 2017 averaged $48. Monthly differences in out-of-pocket insulin spending were more pronounced for people enrolled in consumer-directed health plans (CDHPs) where out-of-pocket spending in January was more than four times spending in December.
Most insurance plans require enrollees to meet a deductible by paying out of pocket for medical services and prescription drugs before the plan will cover these costs. As a result, out-of-pocket spending on covered services and drugs can vary throughout the calendar year, with individuals paying higher amounts at the point of service or sale in January compared to December of the same year. This is particularly true for individuals with chronic conditions that require regular treatment and those in consumer-directed health plans that carry higher deductible amounts. Once the deductible is met, enrollees may still pay a portion of the charges for medical services and prescription drugs out of pocket in the form of co-pays or co-insurance, the amount of which depends on the service or drug and the specifics of their health insurance plan's benefit design.
Figure 1 illustrates this phenomenon in the context of out-of-pocket spending on insulin prescriptions by individuals with employer-sponsored insurance.
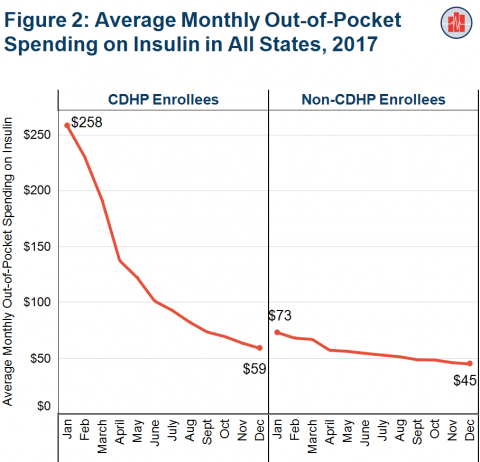
Due to differences in their plans' benefit designs, individuals enrolled in CDHPs can experience more dramatic month-to-month fluctuations in their out-of-pocket spending on insulin relative to those not enrolled in CDHPs. Among individuals enrolled in CDHPs, out-of-pocket spending on insulin averaged $258 in January and $59 in December. By comparison, enrollees in non-CDHPs paid $73 on average in January and $45 on average in December out of pocket on insulin.
The interactive map below shows average monthly out-of-pocket spending by state. To explore, choose the state of interest on the map. (Note, when enough data were not available, no information about out-of-pocket spending on insulin at the state and/or health plan type is displayed.)
Recently, Colorado passed a first-in-the-nation law capping monthly out-of-pocket spending on insulin at $100. Some insurance companies and pharmacy benefit managers, including UCare, Medica and Cigna/Express Scripts, have also announced plans to impose caps for certain members. We calculated the share of enrollees with out-of-pocket spending on insulin above $25, $50, $100, and $200 in each month of the year for those enrolled in CDHPs and non-CDHPs. To explore how these shares vary by state, use the dropdown menu in the dashboard below. For example, among CDHP enrollees in Colorado in HCCI data, the prevalence of monthly out-of-pocket spending on insulin above $100 varied from 45% in January 2017 to 21% in October 2017; among those in non-CDHPs the range was 16% in January 2017 to 7% in November 2017. (Note, when enough data were not available, no information about out-of-pocket spending on insulin at the state and/or health plan type is displayed.)
and Cigna/Express Scripts, have also announced plans to impose caps for certain members. We calculated the share of enrollees with out-of-pocket spending on insulin above $25, $50, $100, and $200 in each month of the year for those enrolled in CDHPs and non-CDHPs. To explore how these shares vary by state, use the dropdown menu in the dashboard below. For example, among CDHP enrollees in Colorado in HCCI data, the prevalence of monthly out-of-pocket spending on insulin above $100 varied from 45% in January 2017 to 21% in October 2017; among those in non-CDHPs the range was 16% in January 2017 to 7% in November 2017. (Note, when enough data were not available, no information about out-of-pocket spending on insulin at the state and/or health plan type is displayed.)
HCCI has been conducting analyses of insulin prices and spending. You can view HCCI insulin research and media coverage on our website.
-
Methods Note
We calculated monthly out-of-pocket spending on fills for prescriptions of all types of insulin products using claims data from the Health Care Cost Institute. Our sample included individuals enrolled in employer-sponsored insurance coverage for at least one month during calendar year 2017, who were under the age of 65, and filled at least two prescriptions for insulin during the year. We did not restrict to individuals with type 1 diabetes. We excluded individuals in the top and bottom 1 percent of insulin use during the year.
Consumer directed health plans are a type of high deductible plan that include either a health savings account (HSA) or a health reimbursement arrangement (HRA).
Out-of-pocket spending is the total amount paid by the patient at the point of sale and includes amounts applied to a deductible, as well as any required co-insurance or co-pay. Average out-of-pocket spending reflects total out-of-pocket spending on all claims filled during a month, divided by the number of unique individuals filling a prescription during the same month. Since not every person fills a prescription every month, the sum of monthly average out-of-pocket spending does not equal annual out-of-pocket spending. Rather, the monthly amounts reflect what the average person who filled a prescription in that month paid out of pocket.
When enough data were not available, the state and/or health plan type have not been included in the figures.
When you subscribe to the blog, we will send you an e-mail when there are new updates on the site so you wouldn't miss them.