COVID-19 testing has become a regular part of life for many Americans over the last two years. In addition to facilitating individual returns to work, school, and other activities, testing is a crucial component of the public health strategy to monitor and address the spread of the virus. Even as testing becomes more available, there is widespread concern and frustration about the high and variable costs of COVID tests. In 2021, at-home tests became more widely used, however even these can be costly (e.g., the current cost of a single antigen rapid test at CVS is approximately $12). These costs and intermittent supply shortages have led to a lack of access at times.
Federal and state policies have aimed to reduce the financial burden of COVID testing for patients by requiring insurance companies to cover tests with no cost-sharing. Yet, even when tests are free to people at the time they get them, when insurers pay high prices for tests, they can pass those costs on to consumers in the form of higher premiums.
To examine the overall and out-of-pocket costs of COVID tests in a population of individuals with employer-sponsored insurance, we used HCCI’s unique commercial claims dataset to analyze claims from over 19 million COVID-19 tests across 50 states and Washington DC in 2020. We also assessed differences in testing rates in rural and non-rural areas among this population, in light of reported variation in access to COVID-19 tests and testing sites (68% of rural counties lacked a testing site, compared to 38% of urban counties).
Per Test Spending on COVID-19 Tests Increased over 2020
As shown in Table 1, average total spending per COVID-19 test rose from $37 in January 2020 to almost $95 per test in July 2020. Total spending is the sum of insurer payments and patient out-of-pocket payments. The most dramatic growth took place between February and March 2020, from $38 to $70. Total spending continued to increase gradually until June, after which spending remained steady at about $95 per test for the remainder of 2020. This trend was driven by an increase in the allowed amount paid by insurers, which increased from $27 in February to $69 in March. In keeping with the goals of federal and state policy, nearly all COVID tests in our data in 2020 had $0 in out-of-pocket costs.
As expected, the testing rate increased significantly over the course of 2020, from 5 tests per 100,000 enrollees in January to 9,631 per 100,000 in December. Given that many individuals received COVID-19 testing outside of the health system and/or not using insurance, it is likely that these data underestimate the number of tests administered over the course of the year. The total number of COVID-19 tests by month in our data, however, is consistent in trend with external benchmarks, such as the COVID-19 Tracking Project at the Atlantic, which suggests the trend and rate in our data are similar to utilization in the general population.
Table 1. National COVID-19 Testing Spending and Utilization, 2020
| Total Spending per Test | Allowed Amount per Test | Out-of-Pocket Cost per Test (not including tests with $0 out-of-pocket) | Out-of-pocket Cost per Test (including tests with $0 out-of-pocket) | % COVID-19 Tests with $0 out-of-pocket | Tests per 100k | |
| January | $37.30 | $25.75 | $11.55 | $22.21 | 48.0% | 5 |
| February | $38.06 | $26.97 | $11.09 | $22.19 | 47.6% | 5 |
| March | $69.96 | $69.23 | $39.53 | $0.73 | 98.2% | 370 |
| April | $78.57 | $78.13 | $46.18 | $0.44 | 99.0% | 965 |
| May | $80.89 | $80.46 | $42.31 | $0.42 | 99.0% | 2,214 |
| June | $92.58 | $92.06 | $57.30 | $0.52 | 99.1% | 3,437 |
| July | $95.19 | $94.82 | $53.74 | $0.37 | 99.3% | 4,917 |
| August | $96.03 | $95.65 | $54.74 | $0.38 | 99.3% | 4,119 |
| September | $95.44 | $95.08 | $53.87 | $0.37 | 99.3% | 4,200 |
| October | $94.37 | $94.02 | $53.77 | $0.35 | 99.3% | 5,837 |
| November | $95.18 | $94.90 | $51.99 | $0.28 | 99.5% | 8,492 |
| December | $94.51 | $92.24 | $48.34 | $0.26 | 99.5% | 9,631 |
Per-Test Spending on and Use of COVID-19 Tests Across States Varied Widely in 2020
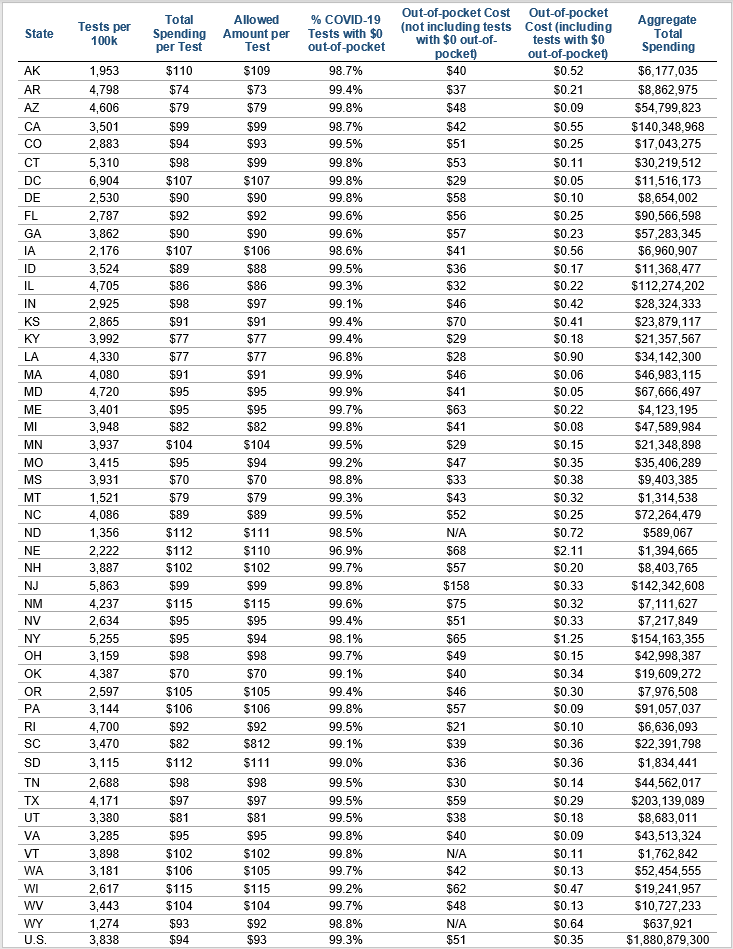
In our data, total national spending in 2020 on COVID-19 tests was close to $1.9 billion. As shown in Table 2, total spending at the state level ranged from $589,000 in North Dakota to $203 million in Texas, reflecting variation in the price of tests and how frequently they were used.
The average total spending per COVID-19 test ranged from $70 in Mississippi to $115 in Wisconsin. In all states, over 95% of COVID tests had $0 in out-of-pocket costs. Among the small percentage of tests with some out-of-pocket costs, the average out-of-pocket dollar amount per test ranged from $20 in Rhode Island to $158 in New Jersey.
There was significant state-level variation in the number of COVID tests per 100,000 individuals in 2020 (Figure 1). Over the year, the testing rate was highest in Washington DC (6,904 per 100,000) and lowest in Wyoming (1,274 per 100,000). As noted above, many COVID-19 tests occurred outside of the insurance system and, therefore, are not captured in our data. The proportion of tests captured in our data likely varies across states depending on where people sought tests, including the availability of free testing (i.e., not resulting in an insurer claim). In some places, people may have been more inclined to seek care outside the health care system due to fears of infection, decreased income, and lack of safe, socially distant transportation.
Table 2. COVID-19 Testing Spending and Utilization by State, 2020
 for Most People in 2020″ class=”wp-image-5962″/>
for Most People in 2020″ class=”wp-image-5962″/>By the End of 2020, the COVID-19 Testing Rate in Rural Areas was 33% Lower than in Non-Rural Areas
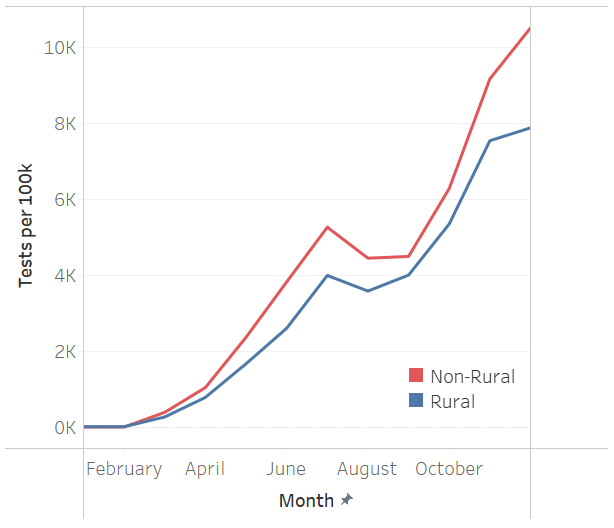
As shown in Figure 2, the testing rate was similar in rural and non-rural areas in January of 2020 (approximately 5 and 14 per 100,000 enrollees, respectively). By the end of the year, however, a gap in test rates between rural and non-rural areas emerged. In December 2020, testing rates were 7,889 per 100,000 in rural areas and 10,523 per 100,000 in non-rural areas.
This trend may reflect several factors, including longer travel times to testing sites. Although the median travel time to a testing site was 20 minutes, early reports suggested that people in rural areas had to travel up to six hours to receive a COVID-19 test. Other factors, including limited information about COVID-19 testing and lack of public transit, may also contribute to differences in testing rates.
Figure 2. COVID-19 Tests per 100,000 Enrollees in Rural and Non-Rural Areas by Month, 2020
 for Most People in 2020″ class=”wp-image-6728″/>
for Most People in 2020″ class=”wp-image-6728″/>Our data show that increases in the COVID testing rate in 2020 were accompanied by virtually no out-of-pocket spending among people with employer-sponsored insurance. Over the same period, insurer costs per test grew, leading to a total of $1.9 billion in spending on tests in 2020. These findings suggest that policies targeting out-of-pocket expenses are working, and policymakers will want to consider the impacts of potentially expiring out-of-pocket protections. Policymakers should also be mindful of how the increase in insurer costs of COVID-19 tests may increase premiums in the future. Throughout the pandemic, insurers have cited the continued cost of COVID-19 testing as one of the most common factors driving up health care costs.
The variation in total spending across states also suggests that there would be substantially different effects of lowered out-of-pocket protections depending on where an individual lives. In turn, we might expect to see less testing in areas with higher out-of-pocket costs, which could have implications for individual and family behaviors as well as overall tracking of COVID-19 case rates.
The ability to use claims data to estimate the number and rate of COVID-19 tests administered is limited since many tests occurred outside the health insurance system (e.g., through drive-through clinics and testing sites) and, increasingly, at home. Further, the extent to which claims data fully represent COVID-19 testing and associated costs is dependent on patient demographics, as well as access to and affordability of COVID testing. Nevertheless, claims data give us one important perspective on trends in testing rates and costs of testing.
