Topics
How often do providers bill out of network?
In recent analysis, we document extensive variation across states and metropolitan areas in the frequency of out-of-network visits among individuals with health insurance provided by an employer. These differences raise the question of whether individual providers bill out of network at dissimilar rates. To explore whether a small group of providers are responsible for most out-of-network billing, or if the practice is widespread, we examined the distribution of out-of-network claims among individual clinicians in 2017. First, we identified visits for emergency medicine, pathology, radiology, anesthesiology, behavioral health, and cardiovascular services performed by providers with the same specialty. Our sample included 13.8 million visits by over 35 thousand unique providers. We then calculated the percent of providers with at least 1 out-of-network claim, as well as the percent of out-of-network claims by provider billing at least once out of network. (Note, unique providers were identified using encrypted provider identification numbers in the HCCI data and may represent either a single clinician, or a group of clinicians that bill under the same provider number.)
Less than half of specialist providers studied bill out of network
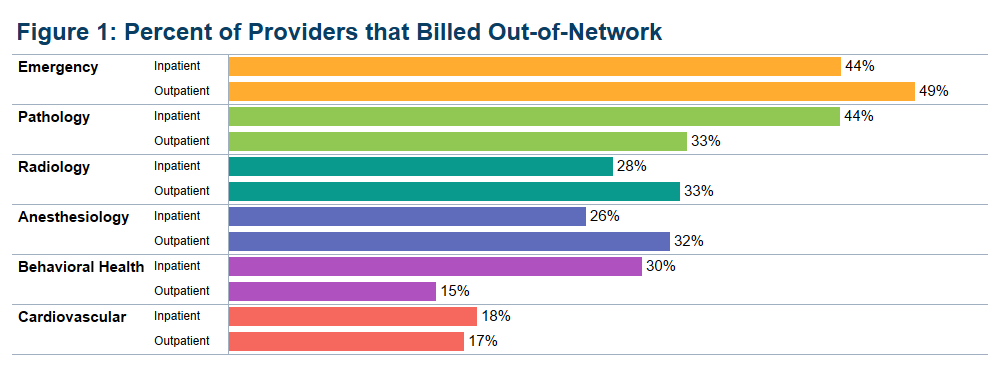
Among providers with one of the specialties we examined, the share with at least one out-of-network claim associated with an in-network inpatient stay ranged from 18 percent for cardiology to 44 percent for emergency medicine. The share of providers with at least one-out-of-network claim associated with an in-network outpatient visit ranged from 15 percent for behavioral health to 49 percent for emergency medicine. The figure below shows the share of providers who billed out-of-network at least once for inpatient and outpatient visits.
Most providers who bill out of network do so less than 10 percent of the time
Among providers with one of the six specialties we examined who billed out of network at least once, we find that within each specialty, the plurality billed out of network less than 10 percent of the time. However, there were some providers within specialties who always, or almost always billed out of network. For instance, 36 percent of pathologists billing out of network for inpatient visits and 20 percent of pathologists billing out of network for outpatient visits did so more than 90 percent of the time. In contrast, virtually no cardiologists billed out of network this often. As shown in the figure below, among other specialties we examined, the share of providers billing out of network more than 90 percent of the time was similar, ranging from 5-8 percent for inpatient visits and 10-16 percent for outpatient visits.
Conclusion
Among six common provider specialties, we found substantial variation in the prevalence of providers who billed out of network. In every specialty, more than half of the sample's providers never billed out of network. And even among providers who did bill out of network, the plurality to vast majority – depending on the specialty - tended to bill out of network infrequently (less than 10 percent of the time). There were, however, some providers who almost exclusively billed out of network (more than 90 percent of the time), most notably in the pathology specialty. Consistent with previous work, these findings show that out-of-network billing practices are not common across providers (see for example, Duffy et. al and Cooper et. al). However, as the flurry of media reports of the last year indicate, those who do receive a surprise bill are often subject to tens of thousands of dollars of unexpected costs. Understanding the variation in how frequently providers bill out-of-network across specialties can help stakeholders craft targeted policy solutions when addressing the adverse effects of out-of-network bills. This is important to ensure that people are not unfairly saddled with medical bills for unknowingly receiving services from an out-of-network provider.
When you subscribe to the blog, we will send you an e-mail when there are new updates on the site so you wouldn't miss them.